Head size
Issues
Wear
Stability
Normal feel of hip
Increased ROM
Wear
Large head
- increase volumetric wear
- less penetrative / linear wear
Small head
- increased linear wear
- decreased volumetric wear
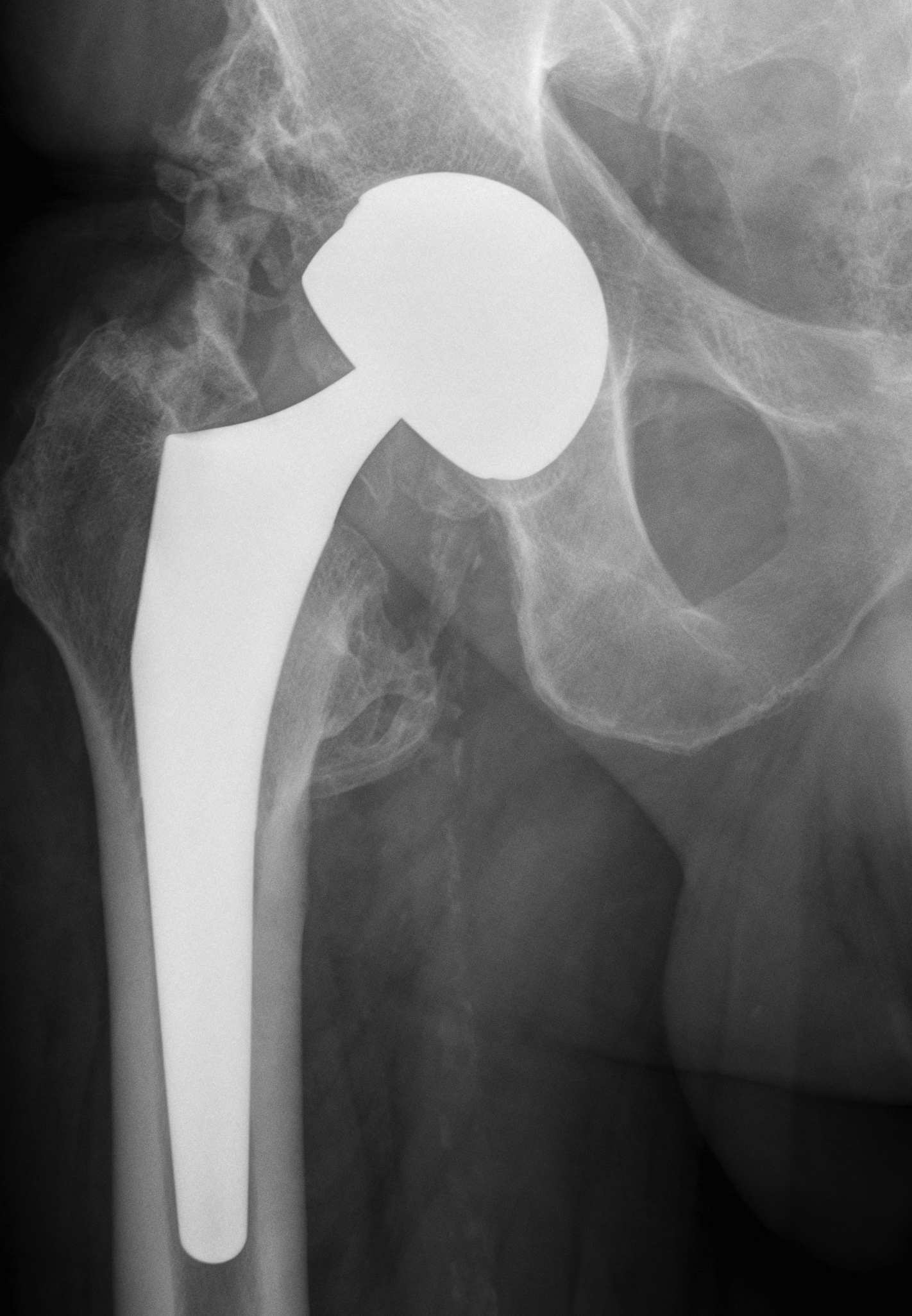
Wear
Stability
Normal feel of hip
Increased ROM
Large head
- increase volumetric wear
- less penetrative / linear wear
Small head
- increased linear wear
- decreased volumetric wear
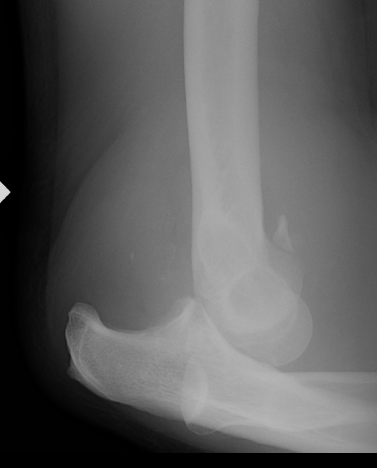
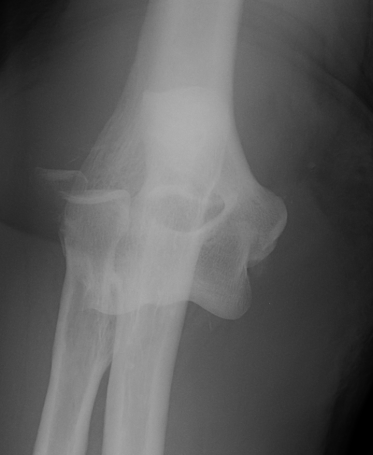
6 /100 000
- second most common dislocation after shoulder
FOOSH
Diagnosis
Pisotriquetral view
- forearm positioned 30° supinated off the neutral position
- loss of symmetry between the pisiform and triquetrum is required for the diagnosis
- carpal tunnel view may be helpful in further assessment of the joint
Clinical
More common problem
Ulna drift & volar dislocation
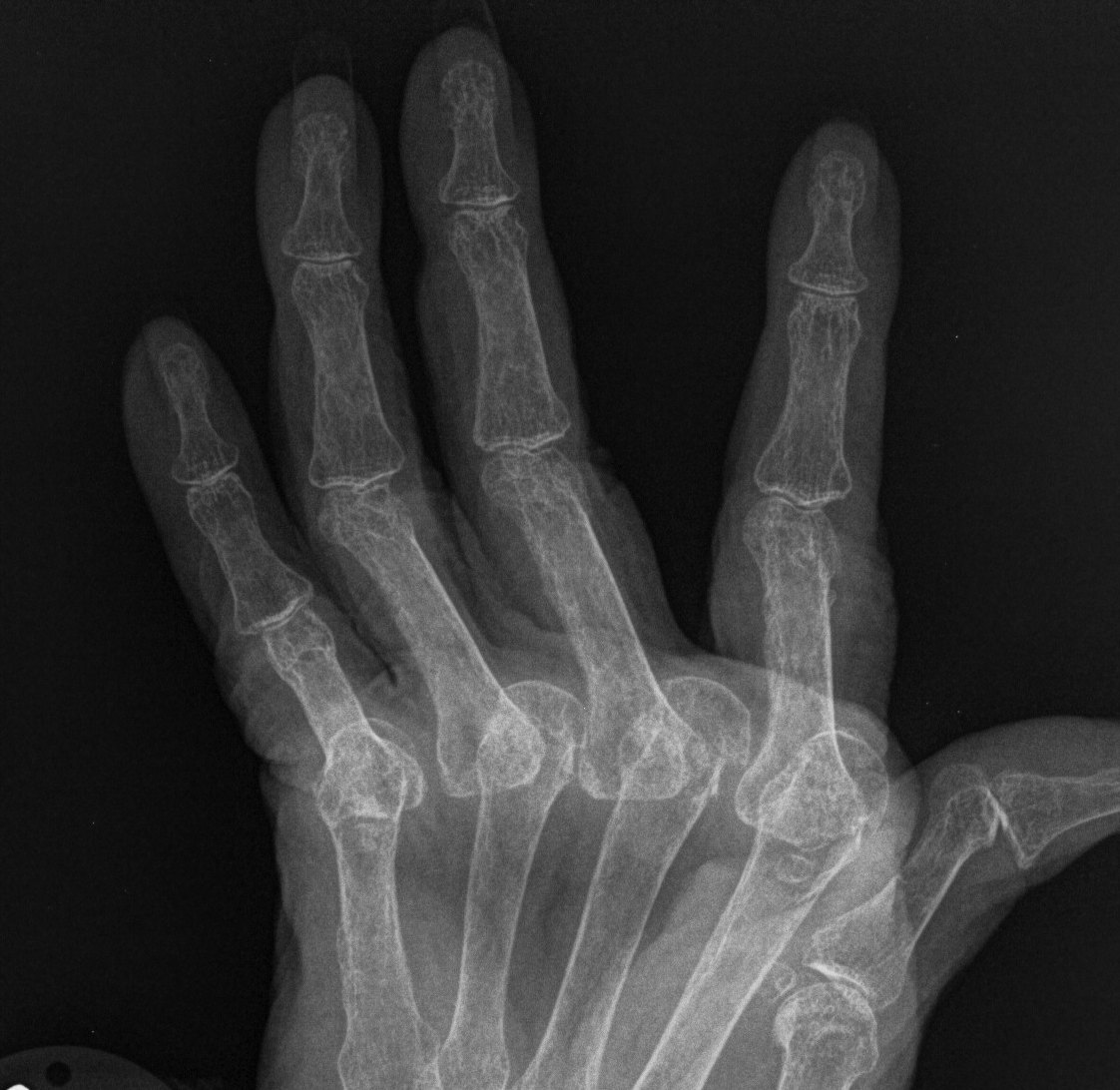
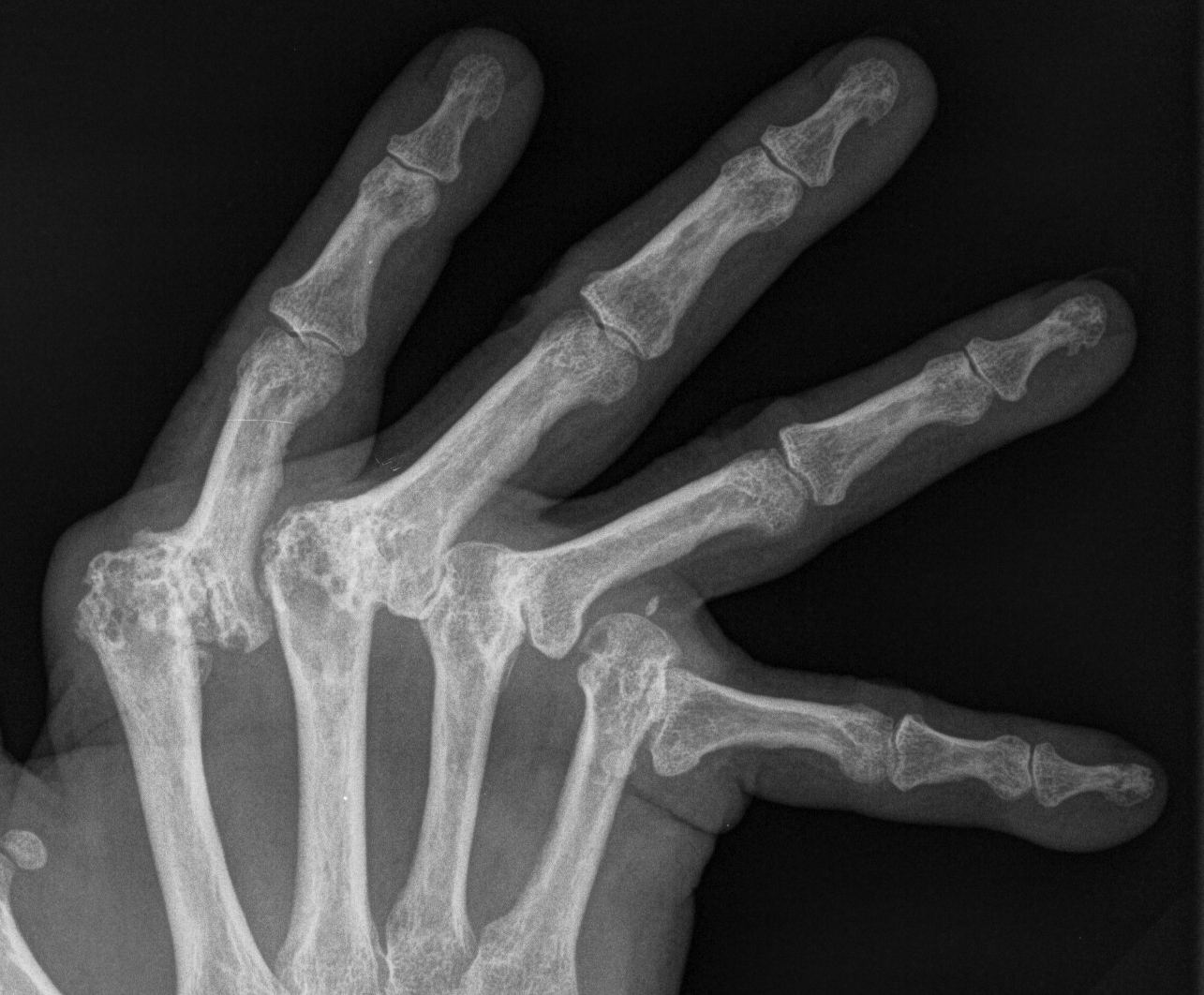
Ulna Drift / Ulna Dislocation
1. Physiological
Patients usually complain of subluxation rather than dislocation
- rarely requires reduction
Different entity to acute posterior dislocation usually
Rare
1. Ligamentous laxity > 50%
- commonly associated with MDI
- posterior only 20%
- posterior & inferior 20%
Rare
- 2% of acute dislocations
Often missed
- < 1/ 52 25%
- < 6/52 25%
- < 6/12 25%
- > 6/12 25%
A GH dislocation which has been missed for a significant period of time
- time period is arbitary
- > 3-6 weeks
Humerus soft and osteoporotic
Significant soft tissue contractures
1. Anterior / subcoracoid dislocation
Beware
- scarring to NV structures
- RC tears including SSC, especially > 40
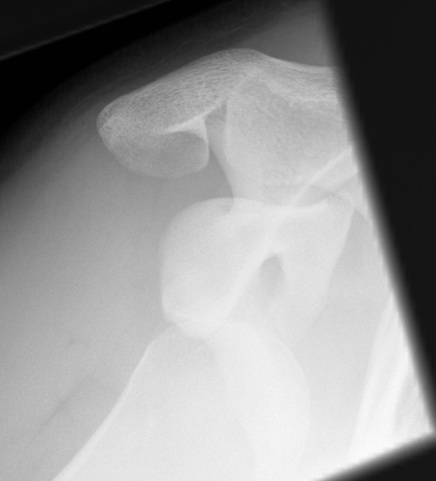
Most common form of shoulder instability
- young males
- M:F = 2:1
Indirect ER and abduction moment on arm
- disruption of anterior stabilisers
Initial injury
- severe pain in shoulder
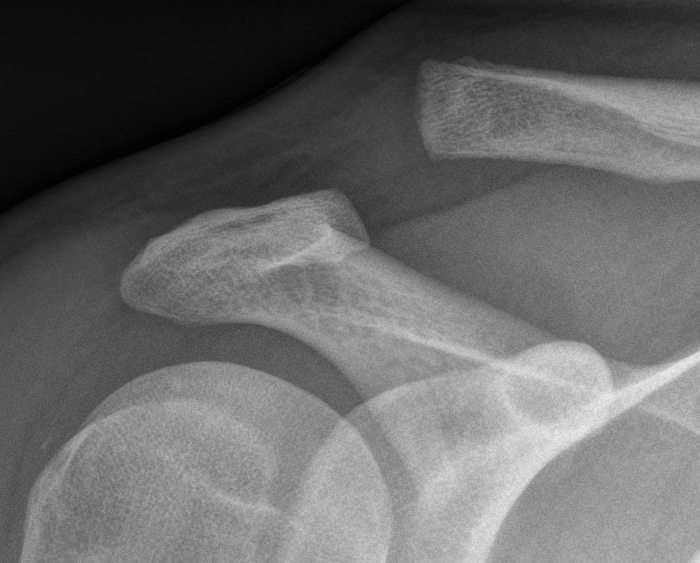
Synovial joint with hyaline cartilage
Has fibrocartilage intra-articular disc
- complete or incomplete
- usually degeneration by 4th decade
Clavicle may lie superior to acromion in normal population
Acromioclavicular Ligaments
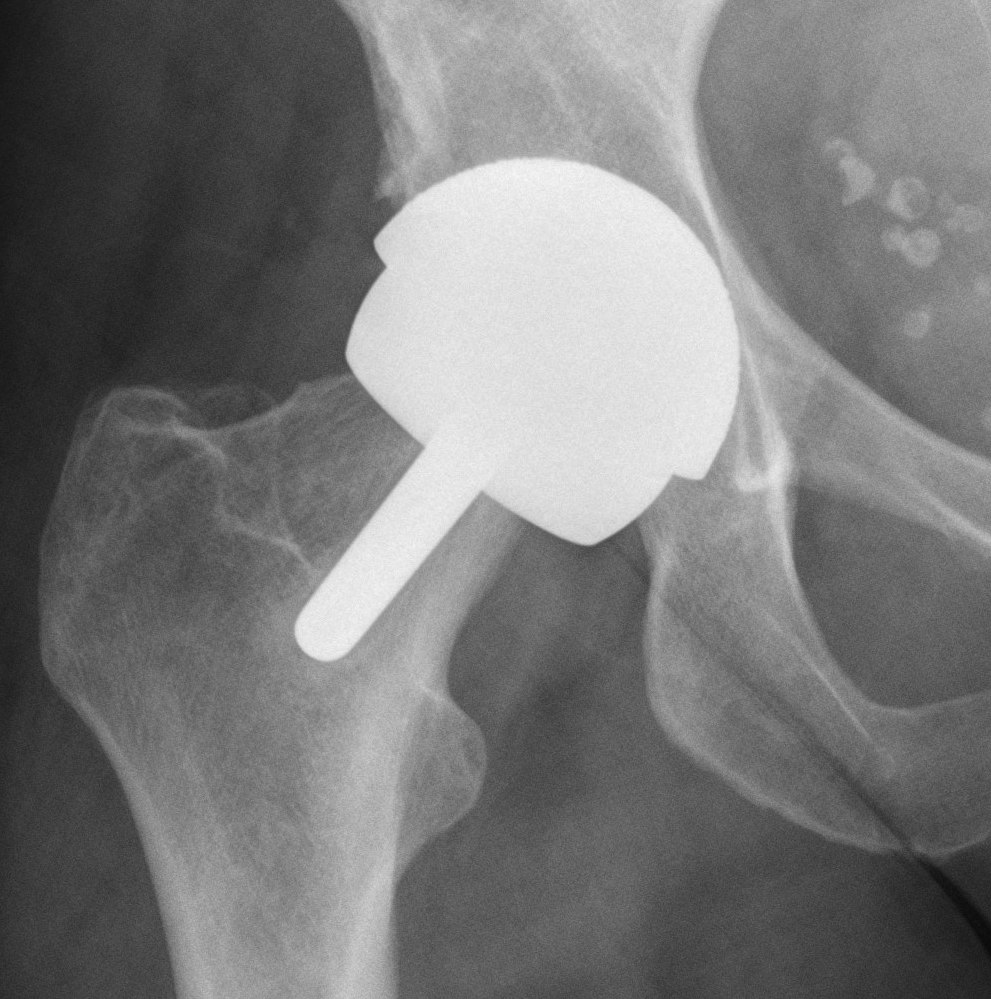
Femur
- removal of femoral head cartilage
- resurfacing with metal
- cemented / uncemented
Acetabulum
- standard technique
Bearing surface
- metal on metal
Relatively young man (40 - 50)
OA